Understanding Meningococcal Disease: What are Meningococci?
Meningococcal disease is a formidable concern for parents and healthcare professionals alike, primarily due to its rapid onset and potential for severe, life-threatening complications such as meningitis (inflammation of the membranes surrounding the brain and spinal cord) or sepsis (blood poisoning). The swift progression of this bacterial infection underscores the critical importance of early recognition and prompt medical intervention to prevent severe outcomes.
At its core, meningococcal disease is caused by bacteria known as *Neisseria meningitidis*, commonly referred to as meningococci. These bacteria typically reside harmlessly in the nasopharynx – the upper part of the throat behind the nose – of a significant portion of the population. In fact, studies suggest that up to ten percent of individuals may carry these bacteria without experiencing any symptoms themselves. Transmission usually occurs through close, direct contact, as the bacteria are delicate and do not survive long outside the human body. Activities like kissing, sharing utensils, or living in close quarters can facilitate the spread of these microbes via respiratory droplets and saliva. While carriage is relatively common, developing an actual invasive infection is thankfully much rarer. Experts explain that in certain, not always understood, circumstances, these bacteria manage to breach the protective mucosal barrier of the nasopharynx, entering the bloodstream and, alarmingly, sometimes even the central nervous system.
Recognizing Meningococcal Infection Symptoms: A Critical Overview
Identifying the symptoms of a meningococcal infection swiftly is paramount, given the disease's aggressive nature. However, this can be challenging because early signs often resemble those of common viral illnesses. The disease typically manifests in two primary forms: meningitis and sepsis, each presenting with a distinct yet overlapping set of symptoms.
For meningitis, which affects the brain and spinal cord lining, key indicators include:
- Sudden high fever: Often the first noticeable sign.
- Severe headache: Can be intense and persistent.
- Stiff neck: A classic, though sometimes later, symptom making it difficult or painful to touch the chin to the chest.
- Sensitivity to light (photophobia): Discomfort or pain when looking at bright lights.
- Confusion or altered mental status: Drowsiness, irritability, or difficulty concentrating.
- Nausea and vomiting: Can occur without other gastrointestinal symptoms.
In infants and young children, symptoms might be less specific and harder to pinpoint. Look for signs like unusual irritability, a high-pitched cry, excessive sleepiness or floppiness, poor feeding, a bulging soft spot (fontanelle) on the head, or seizures.
When the infection progresses to sepsis, a life-threatening blood poisoning, symptoms can be even more insidious and rapid:
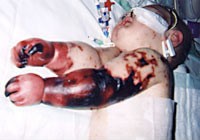
- Rash: A hallmark sign is a non-blanching rash that appears as tiny red or purple spots (petechiae) or larger bruise-like patches (purpura). This rash does not fade when a glass is pressed firmly against it – a crucial "tumbler test" that can help distinguish it from other rashes.
- Cold hands and feet: Even with a high fever, the extremities may feel unusually cold.
- Leg pain: Severe muscle or joint aches, particularly in the legs.
- Pale or mottled skin: A grayish or bluish discoloration of the skin.
- Rapid breathing or shortness of breath.
- Lethargy or unresponsiveness: The individual may become difficult to rouse or appear withdrawn.
It's vital to remember that not all symptoms may appear, and the disease can progress from mild flu-like symptoms to severe illness within hours. If you suspect a meningococcal infection, particularly if a rash appears and doesn't fade under pressure, seek immediate medical attention. Early diagnosis, often involving blood tests and a lumbar puncture to analyze cerebrospinal fluid, followed by swift antibiotic treatment, is critical to improving outcomes and saving lives. For a deeper dive into what to look out for, consult our detailed article on
Meningococcal Infection: Recognizing Early Symptoms and Risks.
Navigating the Diversity: Meningococcal Serogroups and Their Impact
Meningococci are not a single, uniform entity but are categorized into distinct groups, known as serogroups, based on the specific structure of their outer capsule. Scientists have identified twelve such serogroups, designated by letters: A, B, C, E, H, I, K, L, W, X, Y, and Z. However, it's important to understand that not all of these serogroups are equally prone to causing human disease. While many exist, only a handful are consistently linked to invasive meningococcal infections—the ones that cause severe illness by penetrating the body's protective barriers.
Globally, and particularly in regions like Germany, laboratories primarily identify serogroups A, B, C, W, X, and Y as the main culprits behind invasive disease. The prevalence of these serogroups can vary by geographical region and over time, influencing public health strategies and vaccination recommendations. In Germany, according to data from the Robert Koch Institute (RKI), the vast majority of meningococcal diseases are attributed to serogroups B, C, W, and Y. Serogroup B accounts for approximately 60 percent of all cases, making it the most dominant. Serogroup Y follows, responsible for roughly 20 percent of infections, while serogroups W and C each contribute around 10 percent. Other serogroups are considered rare in this context. This detailed understanding of serogroup distribution is fundamental, as it directly informs the development and deployment of targeted vaccines.
Protection Through Prevention: Meningococcal Vaccination Strategies
Given the severe and rapid nature of meningococcal disease, vaccination stands as the most effective strategy for prevention. The availability of vaccines targeting different serogroups has been a monumental step in protecting vulnerable populations, especially infants and young children who are among the most susceptible.
The Standing Committee on Vaccination (STIKO) in Germany, for instance, issues clear recommendations for meningococcal immunization. A key recommendation advises parents to vaccinate their infants against meningococci of serogroup B starting at two months of age. This initial vaccination series is crucial, as infants and toddlers are at a particularly high risk for severe outcomes. Catch-up vaccinations for serogroup B are also recommended up to the fifth birthday, ensuring that children who missed their initial doses can still receive protection. Furthermore, the costs for these recommended vaccinations are typically covered by statutory health insurance in Germany, making them accessible to a wide population.
Beyond serogroup B, vaccines are also available that protect against other prevalent serogroups, specifically A, C, W, and Y. While the provided context focuses on the German recommendation for serogroup B, comprehensive protection often includes these other groups, especially for individuals at increased risk due to travel to endemic areas, certain medical conditions (like absent or dysfunctional spleen, or complement deficiencies), or occupational exposure. Teenagers and young adults are another risk group, particularly those entering communal living situations like university dorms, where close contact can facilitate transmission. For these groups, vaccination against serogroups A, C, W, and Y is often recommended to broaden their immunity. Discussing your child's specific risk factors and the appropriate vaccination schedule with your pediatrician is always the best course of action. This proactive approach ensures tailored protection against the diverse threats posed by meningococcal bacteria. To learn more about specific preventative measures and risk groups, explore our article on
Meningococcal Disease: Prevention, Risk Groups, and Vaccination.
The Importance of Early Action and Medical Consultation
The speed with which meningococcal disease can progress from mild symptoms to a life-threatening condition cannot be overstated. This inherent characteristic makes early action not just important, but absolutely critical for positive outcomes. If you or someone you know exhibits symptoms suggestive of a meningococcal infection—especially a sudden high fever, severe headache, stiff neck, confusion, or a rapidly spreading non-blanching rash—do not hesitate. These are emergency signs that warrant immediate medical attention.
Delaying a visit to the emergency room or calling an ambulance could have severe consequences. Healthcare professionals are trained to recognize the subtle signs of this infection, even when they are non-specific, and can initiate life-saving diagnostic tests and antibiotic treatments without delay. Trusting your instincts and acting quickly is the most important step you can take.
In conclusion, meningococcal disease, while rare, is an extremely serious bacterial infection with the potential for devastating outcomes. Understanding its transmission, being vigilant about the diverse range of
Meningokokken Infektion Symptome (meningococcal infection symptoms), and recognizing the importance of vaccination are key pillars in protecting public health. Through increased awareness, widespread vaccination efforts, and prompt medical response, we can collectively work towards minimizing the impact of this dangerous disease.